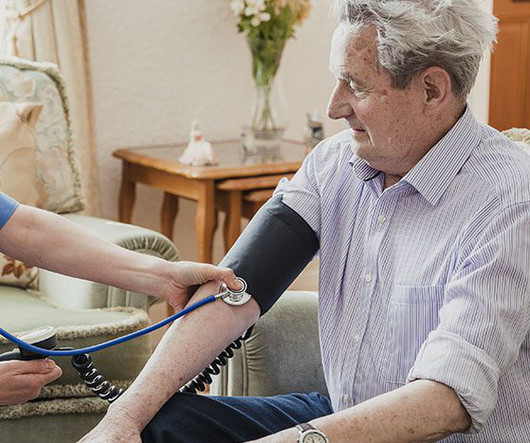
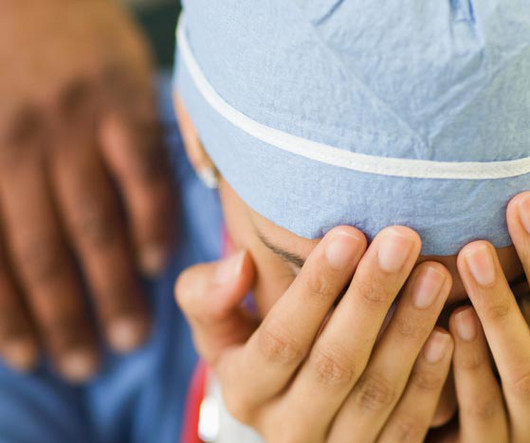
5 Ways to Reduce Horizontal Violence in Healthcare
Relias
SEPTEMBER 20, 2024
Did you know that while only 10% of professionals across industries report experiencing disruptive behavior in the workplace, healthcare professionals report rates that are three times higher? Victims may experience emotional distress, such as anxiety, depression, and low self-esteem.












































Let's personalize your content